What Is Sesamoiditis?
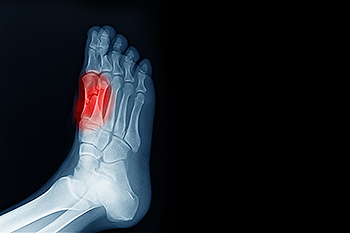
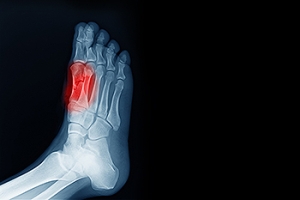
Sesamoiditis is a painful condition involving inflammation of the sesamoid bones, two small bones located beneath the big toe joint. These bones help with movement and bear weight during walking and running. Sesamoiditis is usually caused by repetitive stress, high-impact activities, or wearing shoes that do not provide enough support. Symptoms include pain under the big toe, swelling, bruising, and difficulty bending or straightening the toe. Risk factors include participating in sports like running or dancing, having high arches, or spending long hours on hard surfaces. A podiatrist can diagnose sesamoiditis through examination and imaging, then recommend treatments such as rest, footwear changes, custom orthotics, and stretching exercises to reduce pain and promote healing. If you have pain in this part of your foot, it is suggested that you contact a podiatrist who can accurately diagnose the problem, and offer appropriate relief and treatment solutions.
Sesamoiditis is an unpleasant foot condition characterized by pain in the balls of the feet. If you think you’re struggling with sesamoiditis, contact one of our podiatrists of Apple Podiatry Group. Our doctors will treat your condition thoroughly and effectively.
Sesamoiditis
Sesamoiditis is a condition of the foot that affects the ball of the foot. It is more common in younger people than it is in older people. It can also occur with people who have begun a new exercise program, since their bodies are adjusting to the new physical regimen. Pain may also be caused by the inflammation of tendons surrounding the bones. It is important to seek treatment in its early stages because if you ignore the pain, this condition can lead to more serious problems such as severe irritation and bone fractures.
Causes of Sesamoiditis
- Sudden increase in activity
- Increase in physically strenuous movement without a proper warm up or build up
- Foot structure: those who have smaller, bonier feet or those with a high arch may be more susceptible
Treatment for sesamoiditis is non-invasive and simple. Doctors may recommend a strict rest period where the patient forgoes most physical activity. This will help give the patient time to heal their feet through limited activity. For serious cases, it is best to speak with your doctor to determine a treatment option that will help your specific needs.
If you have any questions please feel free to contact our offices located in Arlington Fort Worth, And Flower Mound, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Sesamoiditis
Sesamoiditis is a condition that affects the joint that is just behind the big toe in the area known as the ball of the foot. It is most common in younger people and people who have just begun an exercise program. Since the sesamoid bones are like a pulley controlling the big toe, they can rub against each other and cause a gradual onset of pain. Pain may also be caused by the inflammation of tendons surrounding the bones. If ignored, sesamoiditis can lead to other, more serious problems such as severe irritation and fractures of the bones.
The cause of sesamoiditis is sudden increase in activity. The ball of your foot acts as a springboard to help you lift off when you are jogging or running. Sudden increase in the use of these bones or the tendon that controls them can cause irritation. The tendon then begins to develop inflammation and the joint begins to swell. People with smaller, bonier feet or those with a high arch are typically more susceptible to this condition.
Sesamoiditis is fairly simple to diagnose since the symptoms have a gradual onset rather than a sudden impact. The symptoms begin with slight irritation around the joint shortly after the increase in activity. The discomfort eventually turns to pain with light swelling and possibly redness. Although redness or bruising are rare, this may be a symptom. After each session of exercising, the aggravated joint becomes more irritated and increases into a very intense throbbing.
Treatment for sesamoiditis can vary depending on the severity of the situation. However, treatment is almost always approached in a noninvasive way. For a case that is just beginning the doctor may recommend a very strict rest period that will limit the activity allowed on the joint. If you must be active, a recommendation for as modified shoe or insole, along with bandaging and immobilizing the big toe will be made to ensure that pressure is not placed on the joint. For severe cases, it is typically recommended that the joint and the big toe be completely immobilized to allow adequate time to heal. Ice and an over the counter anti-inflammatory may can help with the pain and discomfort while you are at rest.
When you return to your regular exercise activities, it is recommended that you use an insole that will allow even distribution of impact to your entire foot, rather than just the balls of your foot. This will prevent further aggravation of the injury.
The Importance of a Diabetic Foot Exam
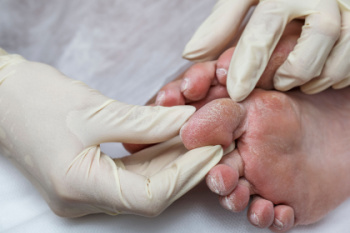
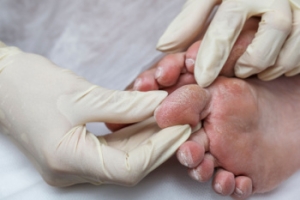
A diabetic foot exam is a comprehensive evaluation of the feet performed to detect early signs of complications related to diabetes. This exam is essential because diabetes can lead to reduced circulation and nerve damage, increasing the risk of foot ulcers, infections, and loss of limb. Causes for needing this exam include prolonged elevated blood sugar levels, poor foot hygiene, and inappropriate footwear. Symptoms that may prompt an exam include numbness, tingling, swelling, changes in skin color, or non-healing wounds. Regular foot exams can help prevent serious complications and ensure early treatment. If you have diabetes, it is strongly suggested that you are under the care of a podiatrist who can perform routine foot evaluations and preserve mobility through proactive and personalized care.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact one of our podiatrists from Apple Podiatry Group. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our offices located in Arlington Fort Worth, And Flower Mound, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetic Foot Conditions
According to the American Diabetes Association (ADA), diabetes is a condition that affects approximately 23.6 million Americans. Around 750,000 new cases are diagnosed each year, and the disease’s most common form, Type 2 diabetes, makes up for 90 to 95 percent of these cases. Type 2 diabetes is especially prevalent among older Americans, those who are obese, and those who lead sedentary lifestyles.
Complications of the disease may lead to several foot and ankle-related conditions. The loss of nerve sensation, or neuropathy, can cause diabetics to lose feeling at the bottom of the feet and therefore leave them unaware of pain, pressure, and heat. Decreased circulation is another complication of diabetes that can slow down the healing of wounds and injuries; this can lead to the development of foot ulcers.
To prevent foot ulcers from forming, diabetics should examine their feet every day for small cuts and wear shoes that curtail pressure. Constant monitoring for the risk factors associated with ulcer formation can allow for early detection and therefore lessen the possibility of ulcers or, even worse, amputation. The removal of calluses and ingrown toenails should be left to the podiatrist to avoid improper removal and possible infection.
Diabetic patients may also experience foot deformities due to complications in their feet, such as limited joint mobility, muscle atrophy, and decreased fat padding. These complications can increase pressure in certain areas of the foot, which in turn can cause certain deformities, such as hammertoe, to form. Another deformity, Charcot foot, develops due to the collapsing of microfractures in the bones of the feet. The resulting deformity is a foot that is flattened and wider in appearance.
To help minimize pressure and prevent the development of these diabetes-related foot and ankle conditions, your podiatrist may consider using orthotics or special shoes. Charcot foot may be treated using walkers, custom orthotic insoles, or non-weight-bearing or rigid weight-bearing casts or braces. In more serious cases, surgery may be considered to treat more developed deformities. Ulcers can be further cared for with the help of proper diet, medication to control glucose, intensive wound care, and infection treatment.
Symptoms a Fractured Ankle
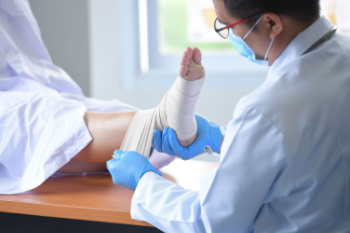
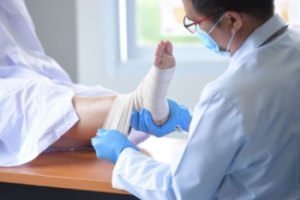
A broken ankle can occur when one or more of the bones in the ankle joint, which include the tibia, fibula, or talus, cracks or breaks due to a fall, collision, or twisting injury. Symptoms of a broken ankle include sudden and intense pain, swelling, bruising, and difficulty in moving the ankle. In many cases, walking becomes impossible, although some people may still bear weight, despite a fracture. A loud snapping sound may be heard at the time of injury. In more severe cases, the ankle may appear misshapen or the broken bone may pierce the skin. A podiatrist can examine the ankle for signs of damage and order imaging tests, such as X-rays, to confirm a fracture. Treatment depends on the location and severity of the break and may involve immobilization with a cast or surgery to realign the bones. Early diagnosis and treatment are important to reduce long-term complications. If you believe you may have fractured an ankle bone, it is suggested that you make an emergency appointment with a podiatrist for an exam and appropriate treatment.
Broken ankles need immediate treatment. If you are seeking treatment, contact one of our podiatrists from Apple Podiatry Group. Our doctors can provide the care you need to keep you pain-free and on your feet.
Broken Ankles
A broken ankle is experienced when a person fractures their tibia or fibula in the lower leg and ankle area. Both of these bones are attached at the bottom of the leg and combine to form what we know to be our ankle.
When a physician is referring to a break of the ankle, he or she is usually referring to a break in the area where the tibia and fibula are joined to create our ankle joint. Ankles are more prone to fractures because the ankle is an area that suffers a lot of pressure and stress. There are some obvious signs when a person experiences a fractured ankle, and the following symptoms may be present.
Symptoms of a Fractured Ankle
- Excessive pain when the area is touched or when any pressure is placed on the ankle
- Swelling around the area
- Bruising of the area
- Area appears to be deformed
If you suspect an ankle fracture, it is recommended to seek treatment as soon as possible. The sooner you have your podiatrist diagnose the fracture, the quicker you’ll be on the way towards recovery.
If you have any questions, please feel free to contact our offices located in Arlington Fort Worth, And Flower Mound, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Broken Ankle Causes, Differences, Symptoms and Treatments
The ankle is a hinged synovial joint made up of three bones: the tibia (shin bone), the fibula (outer ankle bone), and the talus (between the heel and leg). These three bones are bound, supported, and stabilized by strong, fibrous bands of tissue called ligaments.
A break in an ankle bone can be either traumatic or stress related. This injury may be referred to as a break or fracture. A traumatic fracture can result from tripping, twisting or rolling the ankle, falling, or by blunt impact to the ankle. These traumatic ankle breaks usually occur during sporting activities or accidents. Stress fractures, however, occur over time and are the result of repetitive stress to the ankle. These fractures sometimes occur when a new activity that engages the ankle is introduced, or when the level of activity is abruptly increased or intensified.
There are various symptoms that accompany an ankle break. The most significant symptoms are pain and swelling that occurs in the ankle and sometimes spreads up from the foot to below the knee. Bruising or discoloration may develop eventually. It will be difficult or even impossible to put weight on the affected foot, and in severe cases there may be a visible deformity or even exposed bone.
It is very important to seek immediate treatment when an ankle break occurs or is suspected to have occurred, in order to allow the bone to properly heal and to avoid future complications such as stiff joints, limited range of motion, and osteoarthritis.
To diagnose a broken ankle, your podiatrist will first ask you to explain how the injury occurred and what your symptoms are. They will perform a thorough examination, checking for damage to nerves, blood vessels, and other structures around the injury site. They will also test your range of motion. An X-ray will need to be reviewed and, in some cases, an MRI or CT scan may be necessary.
Proper treatment of a broken ankle will depend on where and how severe the break is, how stable the ankle is, and whether the bone is displaced (misaligned or separated) or non-displaced (broken yet still aligned properly).
Mild fractures (where the bone is non-displaced) may be treated by resting, icing, and elevating the ankle at first, followed by immobilization with a cast or walking boot. Pain and inflammation may be treated with acetaminophen. More severe or complicated fractures where bones or joints are displaced may require surgery.
Recovery time will also vary, and it may take 4-6 weeks or longer for a broken ankle to heal. Your podiatrist will most likely order progressive X-rays or stress tests to be taken in order to monitor the healing process.
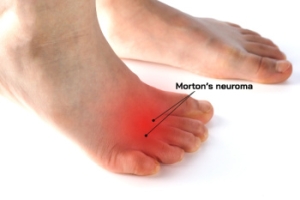
Challenges of Diagnosing Morton's Neuroma

Morton's neuroma is a painful condition involving a thickening of tissue around a nerve in the ball of the foot, often between the third and fourth toes. One of the main challenges in diagnosing it is that the symptoms can mimic other foot problems such as metatarsalgia, stress fractures, or nerve-related issues. People may describe a burning feeling, tingling, or the sense of stepping on a pebble, but the pain may come and go, making it harder to pinpoint. Physical exams and imaging sometimes miss the neuroma, especially in early stages. Patients may go through multiple treatments for the wrong condition before receiving an accurate diagnosis. A thorough evaluation by a podiatrist, including listening closely to symptoms and examining foot structure and pressure points, is essential. If foot pain persists without a clear cause, it is suggested you see a podiatrist for an accurate diagnosis and appropriate treatment.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact one of our podiatrists of Apple Podiatry Group. Our doctors will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact our offices located in Arlington Fort Worth, And Flower Mound, TX . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What is Morton's Neuroma?
Morton’s neuroma, (also referred to as Morton’s metatarsalgia, Morton’s neuralgia, plantar neuroma or intermetatarsal neuroma) is a condition that is caused when the tissue around one of the nerves between your toes begins to thicken. This thickening can result in pain in the ball of the foot. Fortunately, the condition itself is not cancerous.
Morton’s neuroma affects women more often than men with a ratio of 4:1. It tends to target women between the age of 50 and 60, but it can occur in people of all ages. There are some risk factors that may put you at a slightly higher risk of developing the condition. People who often wear narrow or high-heeled shoes are often found to be linked to Morton’s neuroma. Additionally, activities such as running or jogging can put an enormous amount of pressure on the ligament and cause the nerve to thicken.
There usually aren’t any outward symptoms of this condition. A person who has Morton’s neuroma may feel as if they are standing on a pebble in their shoe. They may also feel a tingling or numbness in the toes as well as a burning pain in the ball of their foot that may radiate to their toes.
In order to properly diagnose you, the doctor will press on your foot to feel for a mass or tender spot. He may also do a series of tests such as x-rays, an ultrasound, or an MRI. X-rays are usually done to rule out any other causes for your foot pain such as a stress fracture. Ultrasounds are used to reveal soft tissue abnormalities that may exist, such as neuromas. Your podiatrist may want to use an MRI in order to visualize your soft tissues.
There are three main options for treatment of Morton’s neuroma: Injections, decompression surgery, and removal of the nerve. Injections of steroids into the painful area have been proven to help those with Morton’s neuroma. Decompression surgery has been shown to relieve pressure on the affected nerve by cutting nearby structures such as the ligaments in the foot. Another treatment option would be to surgically remove the growth to provide pain relief.
If you suspect that you have Morton’s neuroma you should make an appointment with your podiatrist right away. You shouldn’t ignore any foot pain that lasts longer than a few days, especially if the pain does not improve.
Benefits of Using Walking Sticks

Using walking sticks can offer important support for people who experience foot, toe, or ankle discomfort during movement. Walking sticks help distribute weight more evenly across the lower body, reducing pressure on painful or unstable areas of the feet and ankles. They can also provide additional stability, which makes it easier to maintain balance and reduces the risk of falls. Walking sticks encourage a more upright posture that leads to better alignment of the feet and ankles while walking. For people recovering from foot or ankle injuries, or managing conditions that cause instability or weakness, a podiatrist may recommend incorporating walking sticks into a treatment plan. By lessening the weight load on affected joints, walking sticks can ease discomfort and promote a more confident, natural stride. Selecting a properly sized walking stick and using it correctly are important steps in preventing further strain. If you experience foot pain when walking, it is suggested that you schedule an appointment with a podiatrist for guidance on using walking sticks.
Exercising your feet regularly with the proper foot wear is a great way to prevent injuries and build strength. If you have any concerns about your feet, contact one of our podiatrists from Apple Podiatry Group. Our doctors can provide the care you need to keep you pain-free and on your feet.
Exercise for Your Feet
Exercise for your feet can help you gain strength, mobility and flexibility in your feet. They say that strengthening your feet can be just as rewarding as strengthening another part of the body. Your feet are very important, and we often forget about them in our daily tasks. But it is because of our feet that are we able to get going and do what we need to. For those of us fortunate enough to not have any foot problems, it is an important gesture to take care of them to ensure good health in the long run.
Some foot health exercises can include ankle pumps, tip-toeing, toe rises, lifting off the floor doing reps and sets, and flexing the toes. It is best to speak with Our doctors to determine an appropriate regimen for your needs. Everyone’s needs and bodies are different, and the activities required to maintain strength in the feet vary from individual to individual.
Once you get into a routine of doing regular exercise, you may notice a difference in your feet and how strong they may become.
If you have any questions please feel free to contact our offices located in Arlington Fort Worth, And Flower Mound, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.